Articles

Productivity and Burnout
Sustaining the Pulse: Navigating Productivity and Well-being in Australian Primary Healthcare.
General practices are the most frequented healthcare services in Australia, with nearly 85 percent of individuals consulting a general practitioner (GP) each year. Amazingly, over 95 percent of these patients consistently visit the same practice, cementing the general practice as a critical fixture in ...

Addressing Non-Billable Work
Non-billable work, consisting of administrative tasks and patient care coordination outside of face-to-face consultations, poses a significant burden on the productivity of Australian General Practitioners (GPs). This article aims to shed light on the effects of non-billable work on GP productivity in Australia and propose three major solutions, with a specific focus on the potential of automation through generative AI, to ...

Streamline Your Medical Practice with MEDILIT
In today's fast-paced healthcare environment, doctors and allied health professionals in Australia face an increasing burden of administrative tasks, particularly when it comes to Medicare-related paperwork. The time-consuming process of generating medical notes ...
The Privacy Act 1988
MEDILIT takes a best practice, proactive approach to privacy and data security, ensuring full compliance with the Privacy Act 1988 and the Australian Privacy Principles (APPs). Privacy is the core tenet underlying all operations.
Privacy:
Privacy is a top priority for MediLit when handling de-identified data.
They take a 'best practice' approach with regular monitoring, updating and evaluating of ...

Computerised History Taking: A Key Driver in Improving Clinical Decision Making and Patient Care
In the increasingly demanding landscape of healthcare, the accuracy and completeness of a patient's medical history are crucial for effective clinical decision-making and avoiding diagnostic errors. Despite its importance, the traditional method of physician-acquired ...

Ambient AI Scribes: Revolutionising Clinical Documentation and Enhancing Healthcare Delivery
The increasing complexity of clinical documentation within electronic medical records (EMR) has been identified as a significant contributor to clinician burnout, negatively impacting the quality of patient care and the physician-patient relationship. In response to this challenge, The Permanent Medical Group (TPMG) implemented ambient artificial intelligence (AI) scribe ...

Balancing AI Benefits and Patient Privacy: A Physician's Guide to Ethical Use of Medical Scribes
The use of real-time transcription services and language models to generate structured notes requires a thoughtful and comprehensive approach to ensure patient trust and compliance with ethical and legal standards. Here are some objective and practical solutions to consider ...
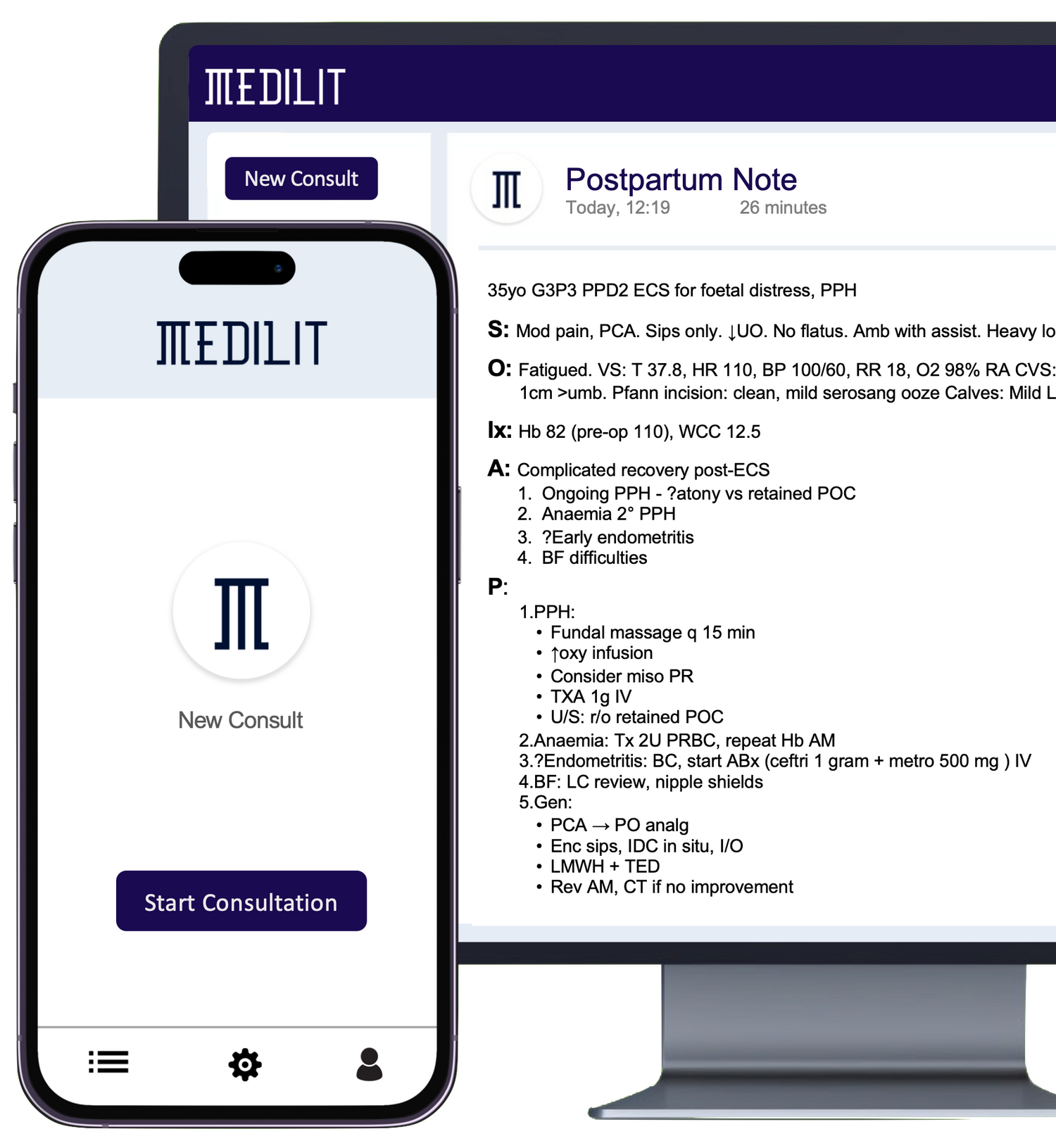
Transforming Australian Healthcare: The Power of AI Scribes
Guardians of Accuracy: AI Scribes Pave the Way for Better Outcomes
Equipped with artificial intelligence, AI scribes play a vital role in ensuring accuracy and efficiency in the Australian healthcare sector. Their capability for precise real-time capture of patient data leads to faster diagnoses and improved treatment protocols, thereby significantly enhancing patient outcomes. A recent study published in the BMC Medical Education journal highlights the potential of AI-powered ...
Transforming Australian Healthcare: The Power of AI Scribes
2 min read
Guardians of Accuracy: AI Scribes Pave the Way for Better Outcomes
Equipped with artificial intelligence, AI scribes play a vital role in ensuring accuracy and efficiency in the Australian healthcare sector. Their capability for precise real-time capture of patient data leads to faster diagnoses and improved treatment protocols, thereby significantly enhancing patient outcomes. A recent study published in the BMC Medical Education journal (https://bmcmededuc.biomedcentral.com/articles/10.1186/s12909-023-04043-4) highlights the potential of AI-powered virtual scribes in medical education, demonstrating their ability to reduce the administrative burden on physicians and improve the quality of patient care.
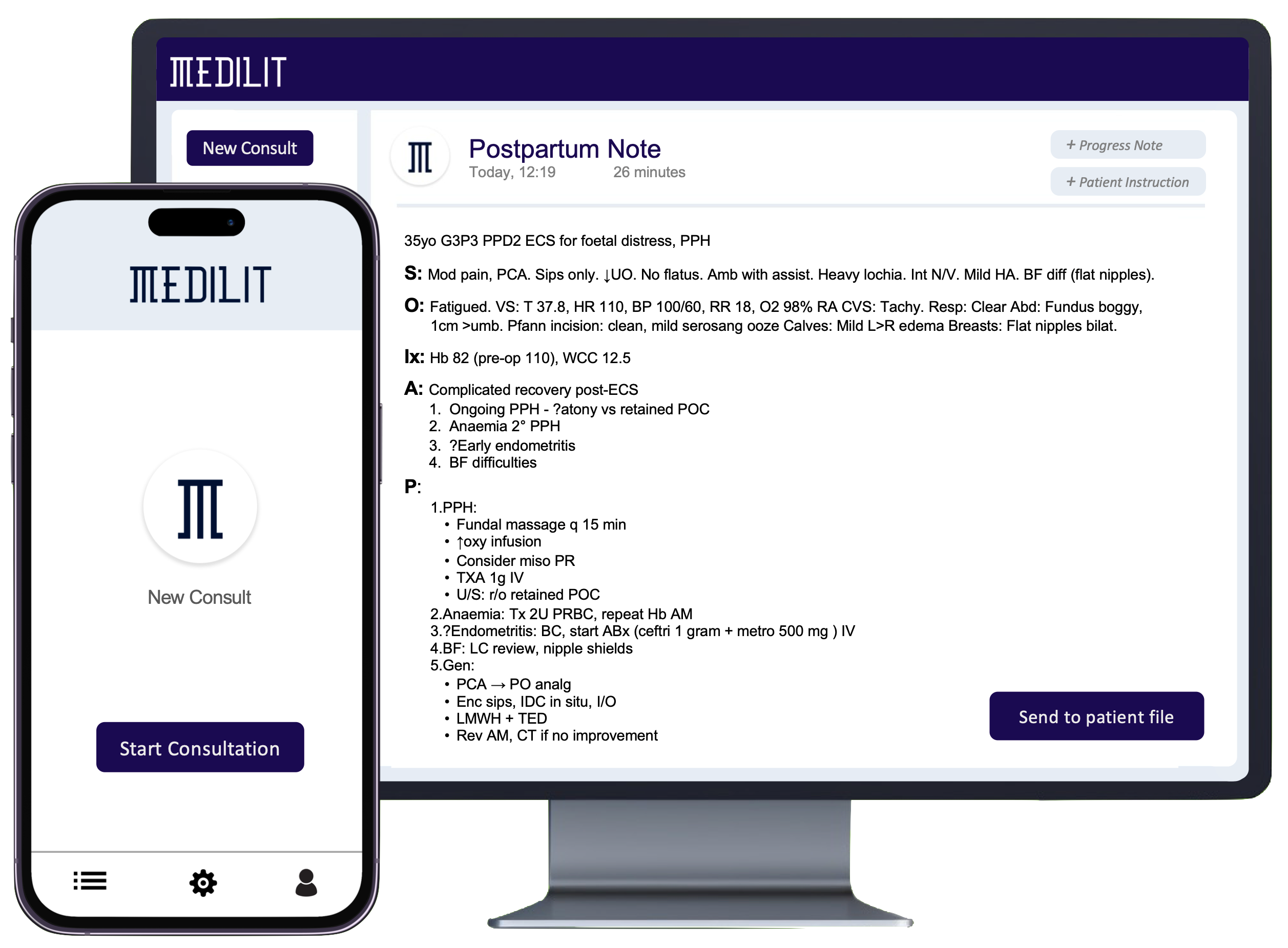
Revitalising Patient Connection: The Human Touch of AI Scribes
One lesser-known yet striking advantage of AI scribes is their contribution to 'rehumanising' healthcare. By managing documentation, AI scribes allow physicians to deepen their engagement with patients. This increase in the empathy quotient plants seeds of satisfaction on both sides of the healthcare equation.Streamlined Operations: AI Scribes as Power Boosters for Australian Healthcare Organisations
For Australian healthcare organisations willing to be at the forefront of innovation, AI scribes offer transformative benefits. From driving efficiencies to cost management and lifting service standards, AI scribes foster a more robust and resilient healthcare landscape across Australia. The University of Adelaide, a leading Australian institution, is actively researching the use of AI assistants to support busy doctors and improve patient care (https://www.adelaide.edu.au/aiml/news/list/2023/11/13/ai-assistant-to-help-busy-doctors-and-their-patients). This demonstrates the growing recognition of AI's potential in the Australian healthcare sector.Bringing Back the Human Element in Healthcare: A Global Perspective
A Harvard Business Review article sees AI as a tool that helps reintegrate the 'human' in human medicine, echoing the valuable shift AI scribes bring to healthcare worldwide, including Australia.Sowing Seeds for the Future: Investing in AI Scribes
Embracing AI scribes offers a pathway to transform the Australian medical field and effectively tackle the crippling issue of physician burnout. Decreased administrative burden, enhanced operational efficiency, and amplified patient interaction collectively help redefine the healthcare model. Early adopters are likely to enjoy the highest Return of investment, moulding a promising horizon for them.Redefining Australian Healthcare: The Necessity of AI Scribes
The advent of AI scribes marks a turning point in Australian healthcare, presenting an exhilarating opportunity to reshape the sector and tackle physician burnout. Let's seize this technological beacon to pave a path towards a more thriving healthcare landscape for both patients and healthcare professionals.
Balancing AI Benefits and Patient Privacy: A Physician's Guide to Ethical Use of Medical Scribes
3 min read
The use of real-time transcription services and language models to generate structured notes requires a thoughtful and comprehensive approach to ensure patient trust and compliance with ethical and legal standards.

Here are some objective and practical solutions to consider:
Informed consent process:
Develop an easily understandable consent form that clearly explains the use of AI in the patient's healthcare journey, including the involvement of transcription services and language models. The consent form should outline the purpose, benefits, and potential limitations of using AI, as well as how patient data will be handled securely.Customisable consent options:
Allow patients to choose which AI-related services they are comfortable with, such as real-time transcription or machine-generated notes. This empowers patients to make informed decisions about their data and ensures that their preferences are respected.Data anonymisation and protection:
Implement state-of-the-art anonymisation techniques to remove personally identifiable information from patient data before it is processed by AI systems. Use robust data protection measures to safeguard patient information during storage and transmission.Service provider agreements and monitoring:
Establish clear data privacy and security agreements with transcription service providers and AI developers. Regularly monitor these providers to ensure adherence to the agreements and maintain the highest standards of data protection.Patient access and data sharing:
Provide patients with secure access to their AI-generated health records and facilitate the seamless and secure sharing of these records with other healthcare providers when authorised by the patient.Physician education and training:
Ensure that physicians are well-informed about the proper use of AI tools, including the importance of obtaining informed consent, safeguarding patient privacy, and accurately interpreting AI-generated insights.Compliance with regulations and guidelines:
Adhere to existing data privacy regulations and stay informed about the development of AI-specific guidelines and best practices. Actively participate in shaping these guidelines to ensure they address the unique challenges posed by AI in healthcare.Continuous patient engagement and improvement:
Actively seek patient feedback on the use of AI in their healthcare experience and address any concerns they may have. Use this feedback to refine AI systems and improve the overall patient experience.
By implementing these solutions, physicians can effectively address data privacy and patient consent issues when using AI-powered medical scribes. This approach ensures that patients remain informed, empowered, and confident in the use of their health data while benefiting from the potential of AI to enhance the quality and efficiency of healthcare delivery.
Ambient AI Scribes: Revolutionising Clinical Documentation and Enhancing Healthcare Delivery
4 min read
The increasing complexity of clinical documentation within electronic medical records (EMR) has been identified as a significant contributor to clinician burnout, negatively impacting the quality of patient care and the physician-patient relationship. In response to this challenge, The Permanente Medical Group (TPMG) implemented ambient artificial intelligence (AI) scribe technology across its network in October 2023, aiming to alleviate the documentation burden on healthcare professionals.

This innovative technology employs machine learning to transcribe clinician-patient encounters in real-time, using smartphones without retaining audio recordings. It promises not only to reduce the time clinicians spend on documentation but also to enhance the quality of patient interactions by allowing physicians to focus more on the patient rather than on data entry tasks.In the initial 10 weeks following implementation, ambient AI scribes were utilised by 3,442 TPMG physicians in over 303,266 patient encounters across various specialties. Early feedback from users has been overwhelmingly positive, with many noting significant improvements in their ability to engage with patients and a reduction in after-hours clerical work. Preliminary assessments indicate that the AI-generated documentation is of high quality, requiring minimal editing by clinicians.Moreover, statistical analyses have shown a link between the use of ambient AI scribes and reduced time spent on documentation and EHR activities. This suggests that ambient AI scribes could play a crucial role in mitigating clinician burnout by streamlining administrative tasks.Despite these promising results, ongoing enhancements are necessary for direct EHR integration, improved medical interpretation capabilities, and personalised workflow options. Additionally, careful attention must be paid to ensure that the technology supports clinicians effectively while maintaining accuracy and relevance in documentation.
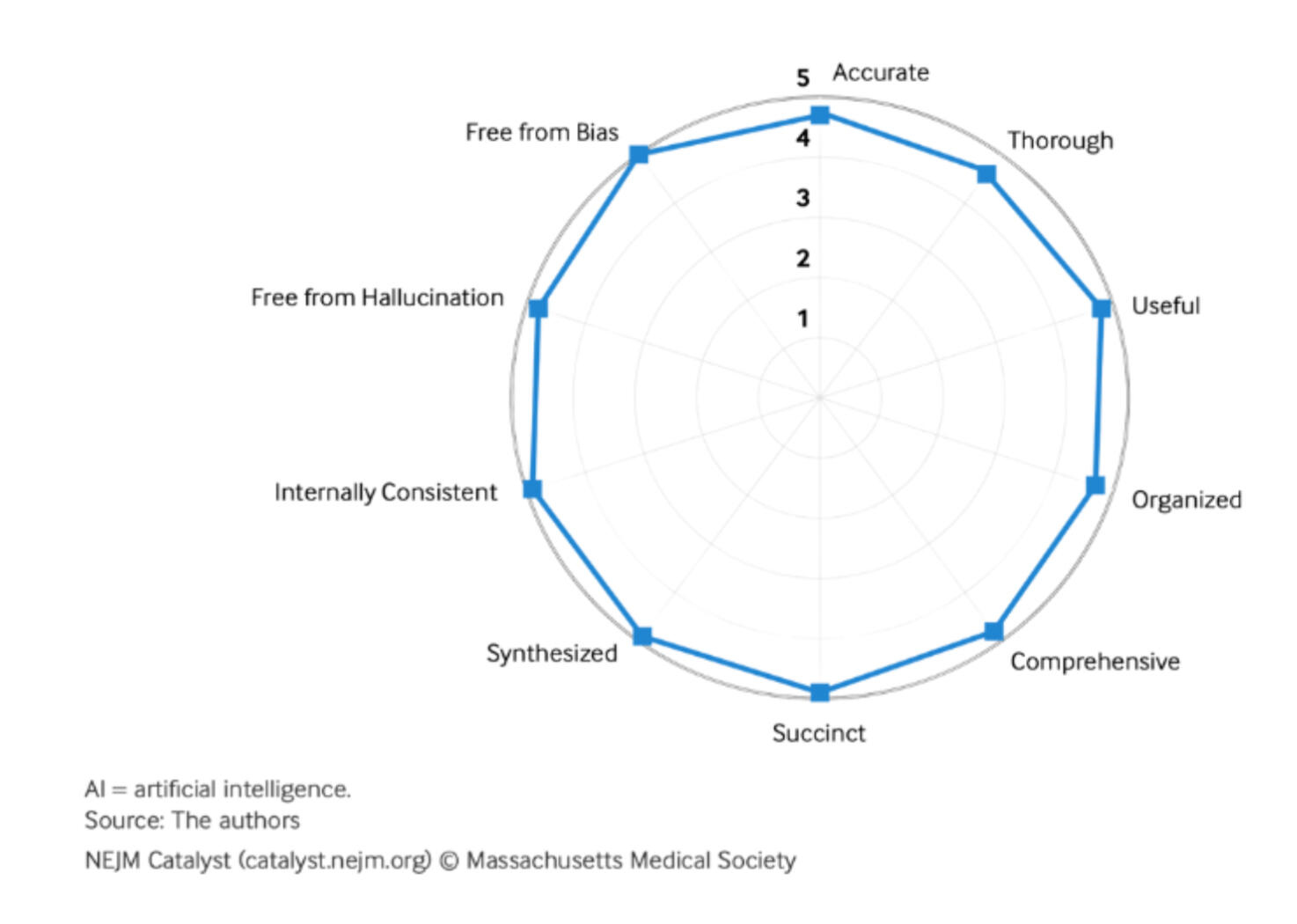
For healthcare organisations considering the adoption of AI-based medical scribe solutions, TPMG's experience underscores the importance of having clinical champions and fostering an organisational culture supportive of innovation. It also highlights the need for a dynamic evaluation framework to assess performance across engagement, effectiveness, quality, and safety domains.In conclusion, ambient AI scribes represent a significant advancement in healthcare technology with the potential to transform clinical documentation processes. By reducing the clerical burden on clinicians and enhancing patient interactions, ambient AI scribes could significantly improve both the efficiency and quality of healthcare delivery.
KEY TAKEAWAYS
Ambient artificial intelligence (AI) scribes show early promise in reducing clinicians’ burden, with a regional pilot noting a reduction in the amount of time spent constructing notes among users.
Ambient AI scribes were found to be acceptable among clinicians and patients, largely improving the experience of both parties, with some physicians noting the transformational nature of the technology in their care.
Although a review of 35 AI-generated transcripts resulted in an average score of 48 of 50 in 10 key domains, AI scribes are not a replacement for clinicians. They can produce inconsistencies that require physicians’ review and editing to ensure that they remain aligned with the physician–patient relationship.
Given the incredible pace of change, building a dynamic evaluation framework is essential to assess the performance of AI scribes across domains including engagement, effectiveness, quality, and safety.
Find more here: https://catalyst.nejm.org/doi/pdf/10.1056/CAT.23.0404
Computerised History Taking: A Key Driver in Improving Clinical Decision Making and Patient Care
4 min read
In the increasingly demanding landscape of healthcare, the accuracy and completeness of a patient's medical history are crucial for effective clinical decision-making and avoiding diagnostic errors. Despite its importance, the traditional method of physician-acquired histories is frequently impacted by time restrictions and subjectivity, leading to potential inaccuracies or incomplete data.

In a recent study, a computerised history-taking (CHT) system was compared with histories documented by physicians in Electronic Health Records (EHRs). Conducted with 410 patients who reported to the emergency department with acute chest pain, the study unearthed some noteworthy advantages of CHT systems:Time-Efficient:
By allowing patients to directly input their historical data, CHT systems can save crucial physician time, which can be better spent on consultations.Comprehensive Assessments:
Through a series of interactive patient questionnaires, CHT systems can amass detailed symptom inventories, which in turn refine differential diagnoses.Accuracy and Completeness:
As the question flows in CHT systems are standardised, they leave no stone unturned, guaranteeing comprehensive and accurate patient histories.Patient Engagement:
By entering their own details, patients can gain a better understanding of their conditions and the importance of providing accurate information.Superior Data Analysis:
Thanks to AI capabilities, CHT systems can detect patterns, assisting in both individual clinical decision-making and overall healthcare planning strategies.
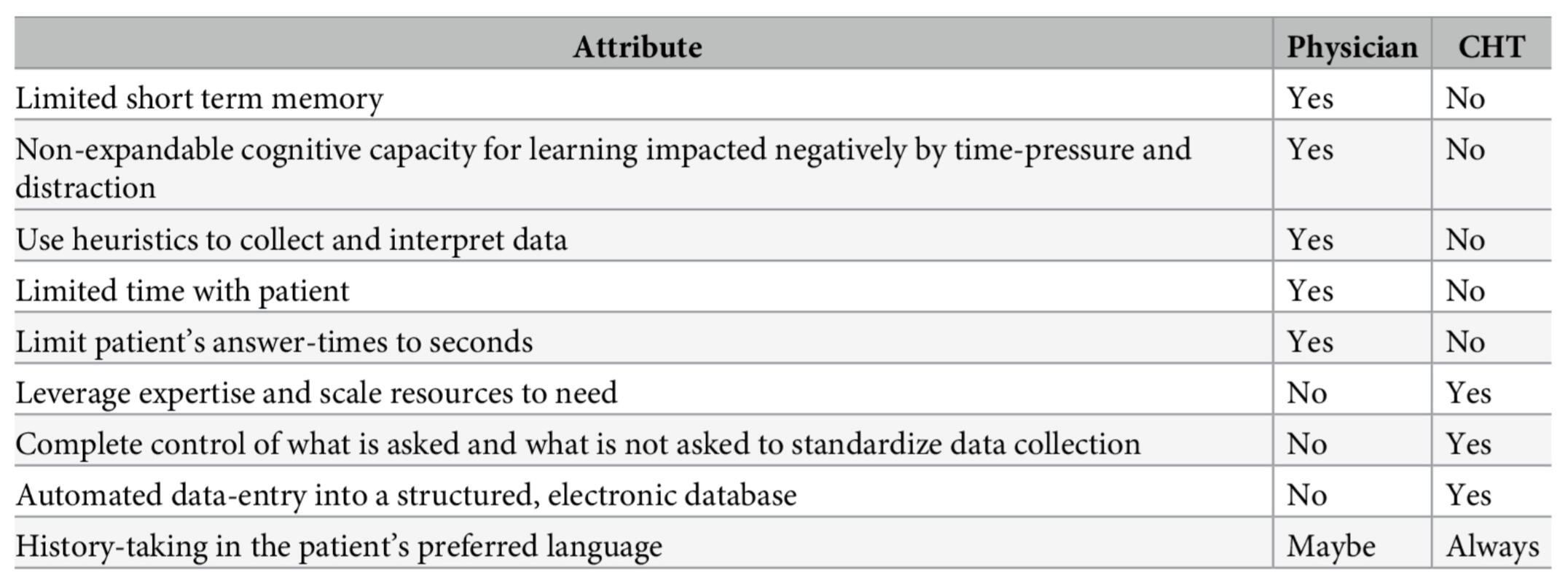
Comparison of physician and CHT attributes affecting the completeness, accuracy and bias of data collected by each method for history-taking.(https://doi.org/10.1371/journal.pone.0257677)
Despite the multiple benefits, it's vital to remember the irreplaceable value of human touch in medicine. CHT systems are best utilised as supplementary tools, enhancing rather than replacing the work of skilled physicians.
In situations assessing critical symptoms such as chest pain, CHT systems offer a potentially life-saving evolution in efficiency and patient care. As technology progresses, healthcare professionals need to weave these digital tools into their practice, aiming to consistently deliver patient-centred, top-tier, efficient care, while preserving the essential human aspect of clinical medicine.Find more here: https://doi.org/10.1371/journal.pone.0257677
The Privacy Act 1988
3 min read
MEDILIT takes a best practice, proactive approach to privacy and data security, ensuring full compliance with the Privacy Act 1988 and the Australian Privacy Principles (APPs). Privacy is the core tenet underlying all operations.
Privacy:
Privacy is a top priority for Medilit when handling de-identified data.
They take a 'best practice' approach with regular monitoring, updating and evaluating of privacy processes and systems.
MEDILIT underwent a third-party Privacy Impact Assessment by a specialist privacy consulting firm.
Their Privacy Management Framework embeds a culture of privacy compliance, establishes robust processes, enables continuous evaluation, and enhances responses to privacy issues.
Privacy processes and systems are transparent and communicated to partners.
They have a comprehensive MEDILIT Privacy Policy accessible publicly.Physical Security:
Infrastructure is co-located in highly secure and certified Australian data centre facilities with stringent physical security controls like 24/7 guards, biometrics, CCTV monitoring, access restrictions etc.
Data centres are located in Australia and certified for PCI-DSS, SOC, ISO 27001 among other standards.Data Security & Access Control:
Systems processing de-identified data are treated as highly sensitive.
Role-Based Access Control restricts user privileges to minimum required for their role.
Employee access is closely monitored and subject to change control mechanisms.
Hard drives/assets are securely erased before decommissioning.Encryption:
Data encryption is employed across all communication paths and at rest.Security Monitoring:
Security team utilises monitoring and analytics to detect malicious activity.
User/system behaviours are monitored and supported by incident response procedures.Network Resilience:
Network designed with redundancy across internet services, firewalls, storage and computing systems.Firewalls & Access Logging:
Next-Generation and Web Application Firewalls control network traffic.
Logging and monitoring of all network and application access activities.Collection of Personal Information (APP 3)
MEDILIT does not collect or store any patient information or personal data through its APIs or platform.
MEDILIT employs robust de-identification techniques, including removing all direct identifiers (e.g., names, contact details) and applying data masking, pseudonymisation, and other privacy-enhancing methods. This ensures that no personal information is processed or stored within MEDILIT's systems, keeping patient confidentiality and safety at the core of its platform.Use and Disclosure of Personal Information (APPs 6 and 8)
As MEDILIT does not collect or store any personal information, there is no risk of unauthorised use or disclosure of such information. The de-identified data processed through MEDILIT's APIs is used solely for the purpose of providing AI-powered analysis, recommendations, and services to healthcare providers and individuals, without any ability to re-identify or trace the data back to specific individuals.Data Quality and Security (APPs 10 and 11)
MEDILIT implements industry-standard security measures, such as encryption, access controls, and regular security audits, to protect the de-identified data it processes from misuse, interference, loss, unauthorised access, modification, or disclosure. MEDILIT does not store any patient data or personal information.
All APIs are in Australia and no data leaves the Australian border.Privacy Policy and Notification (APP 1)
MEDILIT's privacy policy clearly outlines its commitment to patient confidentiality and the de-identification methods employed to ensure no personal information is processed or stored within its systems. This policy is readily available to healthcare providers, individuals, and regulatory authorities.Data Breach Notification
As MEDILIT does not collect or store any personal information or patient data, there is no risk of an eligible data breach involving such information. However, MEDILIT has robust incident response and notification protocols in place to address any potential security incidents involving the de-identified data it processes.By implementing these strict de-identification and privacy-enhancing measures, including encryption and other security controls, and by ensuring all APIs are in Australia with no data leaving the border, MEDILIT ensures compliance with the Privacy Act 1988 and maintains the highest standards of patient confidentiality and safety within its AI software and APIs.
Streamline Your Medical Practice with MediLit:
Alleviating the Burden of Medicare Paperwork
3 min read
IntroductionIn today's fast-paced healthcare environment, doctors and allied health professionals in Australia face an increasing burden of administrative tasks, particularly when it comes to Medicare-related paperwork. The time-consuming process of generating medical notes, completing GPMPs (General Practitioner Management Plans), GPMHCPs (General Practitioner Mental Health Care Plans), CVCs (Chronic Disease Management plans), referral letters, and various certificates can lead to burnout and hinder the delivery of quality patient care. Fortunately, there is a solution – MEDILIT.

The Burnout Epidemic
According to recent studies conducted by leading Australian medical associations, such as the Australian Medical Association (AMA) and the Royal Australian College of General Practitioners (RACGP), excessive paperwork is one of the primary causes contributing to physician burnout. In fact, 65% of doctors reported feeling overwhelmed by administrative tasks associated with Medicare claims processing alone.
Introducing MEDILIT
MEDILIT is an innovative AI-powered platform designed specifically for healthcare professionals in Australia. It offers a comprehensive suite of features that streamline medical note generation and automate tedious paperwork processes related to GPMPs, GPMHCPs, CVCs, referral letters, work cover certificates, Centrelink certificates, and DVA-related documentation.
Benefits for Healthcare Professionals1. Time-saving Efficiency:
By automating repetitive administrative tasks through intelligent algorithms, MEDILIT significantly reduces the time spent on generating medical notes and completing paperwork. This allows doctors more time for their core responsibilities, providing exceptional patient care.2. Increased Revenue Potential:
With its ability to optimise billing codes based on clinical documentation inputs, MEDILIT ensures accurate claim submissions which can potentially increase revenue streams for healthcare practices.3. Work-Life Balance:
By alleviating physicians' burdensome workload associated with paperwork,MEDILIT helps restore work-life balance. Healthcare professionals can now focus on their personal interests and spend more quality time with family and friends.4. Data-driven Insights:
MEDILIT provides valuable analytics and reporting features, allowing healthcare professionals to gain insights into patient demographics, disease prevalence, treatment outcomes, and billing patterns. These data-driven insights enable informed decision-making for improved practice management.
ConclusionMEDILIT is revolutionising the way doctors and allied health professionals manage Medicare-related paperwork in Australia. By leveraging AI technology, this platform offers a comprehensive solution that not only reduces administrative burdens but also enhances efficiency, increases revenue potential,and improves work-life balance. Join the growing community of healthcare professionals who have embraced MEDILIT to streamline their medical practices while delivering exceptional patient care.
Disclaimer:
MEDILIT acknowledges the expertise of healthcare professionals in providing quality care to patients. Our platform aims to support these efforts by simplifying administrative tasks; however, it does not replace professional judgment or clinical decision-making processes.
Addressing Non-Billable Work and Enhancing GP Productivity in Australia
The Potential of Automation through Generative AI
3 min read
IntroductionNon-billable work, consisting of administrative tasks and patient care coordination outside of face-to-face consultations, poses a significant burden on the productivity of Australian General Practitioners (GPs). This article aims to shed light on the effects of non-billable work on GP productivity in Australia and propose three major solutions, with a specific focus on the potential of automation through generative AI, to help alleviate this burden.

Effects of Non-Billable Work on GP Productivity1. Time and Resource Constraints:
GPs spend a significant portion of their time on non-billable work, estimated at around 20%. This reduces the time available for direct patient care, potentially impacting timely access to healthcare services and practice revenue.2. Administrative Burden:
The Australian Medical Association (AMA) acknowledges the administrative workload as a missed opportunity for over 14 million face-to-face consultations annually. Additionally, high administrative burdens are linked to lower job satisfaction among physicians and the likelihood of considering seeing fewer patients in the future.3. Variances with Practice and Practitioner Characteristics:
Limited information exists regarding the variations in non-billable work among Australian GPs based on practice and practitioner characteristics. Understanding these variances is crucial in tailoring effective solutions.
Proposed Solutions1. Automation through Generative AI:
Implementing automation solutions powered by generative AI technology can significantly reduce the time spent on administrative tasks. AI-powered systems can automate paperwork, data entry, appointment scheduling, and even assist in care coordination, allowing GPs to focus more on direct patient care.2. Electronic Health Record (EHR) Optimisation:
Enhancing the functionality and efficiency of EHR systems can streamline documentation processes and improve information management. AI algorithms can help extract and categorise relevant patient data, saving GPs time and enhancing overall productivity.3. Virtual Assistants and Chatbots:
Introducing virtual assistants and chatbots can provide support in administrative tasks, appointment management, and patient communication. AI-powered chatbots can handle routine inquiries and provide information, freeing up GPs' time and improving patient experience.
The Potential of Automation through Generative AIAutomation using generative AI holds immense potential in relieving GPs from non-billable work burdens and enhancing productivity. By leveraging AI algorithms, natural language processing, and machine learning, generative AI systems can analyse vast amounts of data, automate complex administrative tasks, and support GPs in decision-making processes.Benefits of automation through generative AI include increased accuracy, accelerated data processing, reduced human error, and improved patient outcomes. GPs can optimize their time and focus on clinical care, leading to higher job satisfaction and enhanced patient experience.
Productivity and Burnout
3 min read
General practices are the most frequented healthcare services in Australia, with nearly 85 percent of individuals consulting a general practitioner (GP) each year. Amazingly, over 95 percent of these patients consistently visit the same practice, cementing the general practice as a critical fixture in the landscape of Australian healthcare. Despite being heavily utilised and supported by research emphasising the need for a well-funded general practice sector, such services account for a major 7.7 percent of total government health expenditure. The underfunding issue is further exacerbated by the Medicare Benefits Scheme (MBS), which consistently undervalues proper GP services amid inadequate indexation and a rigid consultation item structure.

Central to the discourse presented in the sixth annual report (Health of a nation, RACGP, Nov2023) is a theme that resonates across the field: the sustainability of general practice. Amidst increasing pressures such as unmanageable workloads and administrative burdens, coupled with inadequate remuneration, the sustainability of this sector hangs in the balance. The sheer intensity of these stressors has prompted an alarming trend; more general practitioners including emerging talents from younger cohorts are scaling back their hours, with some contemplating early retirement, thereby expediting the onset of a predicted shortage in the general practice workforce.Burnout, illustrative of the immense strain on individuals, is a phenomenon reported by an overwhelming 73% of general practitioners within the past year alone, signaling a wake-up call to address their well-being and to safeguard the future of primary healthcare delivery. Foremost among the concerns raised is the burgeoning challenge of managing clinical workloads, a stress factor that, for the first time, supersedes the challenge of managing income— and is intricately linked with navigating the ever-tightening labyrinth of regulatory changes.Indeed, nearly half of surveyed GPs have conceded that the financial model underpinning their practice is unsustainable, with many opting to bulk bill out of consideration for their patients' affordability, despite personal financial detriment. Moreover, compliance with Medicare concerns and the complexity attached to it have been reported to substantially divert time from patient care, fostering a climate of apprehension and caution which may inadvertently hinder the provision of services due to fears of compliance repercussions.It is somewhat concerning that government funding has not aligned proportionately with the vital role general practices play. Current funding levels may leave one with the impression that health authorities are content to lean heavily on the intrinsic sense of duty that has long characterised the medical profession.While general practices are under pressure, a window of opportunity is open to reinvent and reinvigorate the system. Let’s start a meaningful dialogue and drive the innovation needed in healthcare. Connect, contribute, and let's navigate towards a smarter, sustainable future in Australian healthcare together.
